Eye Problems May Be Early GPA Symptom; Rituxan Helps in Recurrent Cases
Written by |
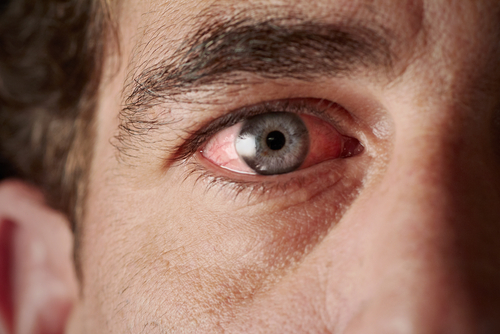
Eye problems are a common symptom of granulomatosis with polyangiitis, of which clinicians should be aware as it can be an initial symptom of the disease, a study reports.
Most of the time these manifestations are treatable by conventional immunosuppressive therapy. But for cases where problems are recurrent or do not respond to treatment, Rituxan (rituximab) seems to be beneficial, leading to a high rate of remission.
The study, “Ocular involvement in granulomatosis with polyangiitis: A single-center cohort study on 63 patients,” was published in the journal Autoimmunity Reviews.
Granulomatosis with polyangiitis (GPA) is a type of ANCA-associated vasculitis marked by blood vessel inflammation of the respiratory tract and lungs. However, patients with this disease may develop other clinical manifestations.
Because of that, clinicians “must be aware of the different manifestations of this disease to avoid a diagnostic delay” and start appropriate therapy early, researchers stated.
One of the other symptoms of GPA is eye inflammation. It is common for patients to note vision problems, eye redness, burning, or pain. In some cases, eye problems can be the first sign of disease.
In this study, researchers analyzed a group of GPA patients referred to the National Referral Center for Vasculitis, Cochin Hospital, in France, to investigate the type of eye manifestations they had, how they were treated, and what the outcome was.
In the 308 GPA patients studied, there was a prevalence of 38.6% (119 patients) of eye manifestations related to the disease.
From this group, 63 patients were selected for further analysis. Their medical records were reviewed, with follow-up data available for a median of 50.5 months.
Analysis revealed that the most common eye disorders were scleritis (26.8%), episcleritis (26.8%), followed by disease of the eye socket, called orbital disease (20.6%).
Scleritis is inflammation of the white, tough coating of the eye, called the sclera. Episcleritis refers to inflammation of the tissue lying between the sclera and the lining of inner eyelids and sclera. Those problems affected both eyes in 29.1% of the patients and resulted in loss of visual acuity in 16.7% of them.
Most of the time (57.1% of the patients) GPA onset was accompanied by an eye disorder together with other broader, or systemic, symptoms (e.g. lung and kidney involvement). However, in a few patients (14.3%), an eye problem was the first sign of the disease. For the other 28.6%, eye disorders only appeared later on.
In most cases, doctors prescribed treatment for GPA due to the patients’ systemic problems, although in 19.0% of the subjects that indication was suggested due to an eye manifestation.
Most (80.9%) resolved with conventional immunosuppressive therapy (corticosteroids, cyclophosphamide, azathriopine or methotrexate) in six to 12 months. In the remaining 19.1%, symptoms persisted or worsened.
In those whose eye disease was recurrent or did not respond to initial treatment, Rituxan (rituximab) was the most commonly chosen therapy to achieve remission.
The medicine seemed to be useful for this group of patients; it led to symptom disappearance in 91.7% of the cases, compared to 72.3% of those taking cyclophosphamide.
Considering the results, researchers stated that eye involvement is not uncommon in GPA, but may be under-recognized, especially when it is the first symptom of the disease.
“Clinicians must be aware of this involvement, since it reflects activity of GPA and requires systemic immunosuppressive drugs to control the symptoms,” they stated.
Rituxan “appears to be a useful tool in inducing remission and controlling relapses” in these patients and when cyclophosphamide fails to control the eye manifestations, they added.


