ANCA-associated vasculitis diagnosis
Anti-neutrophil cytoplasmic antibody (ANCA)-associated vasculitis (AAV) is a group of diseases marked by mistaken immune attacks on small blood vessels. While prompt AAV diagnosis and treatment are important for a better long-term outlook, the disease can be difficult to identify because its symptoms vary widely.
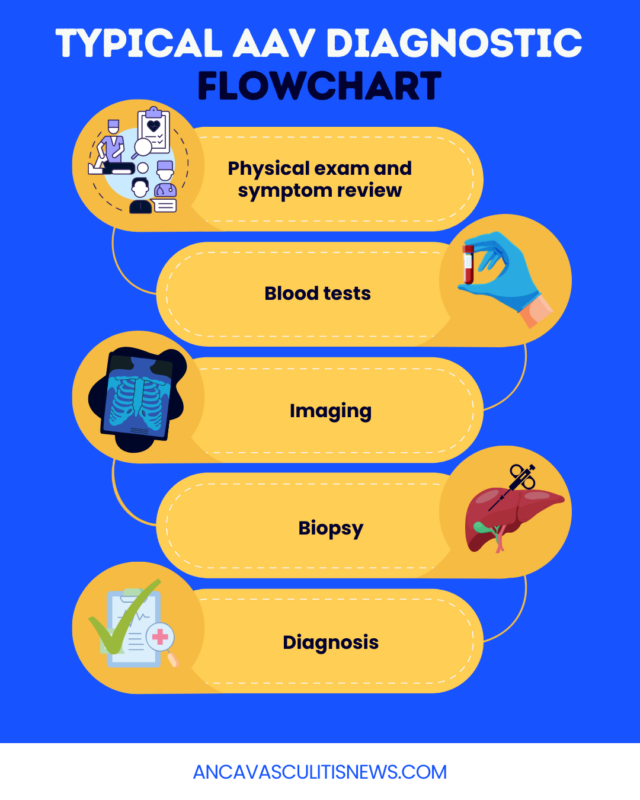
There are no universally accepted diagnostic criteria or definitive tests for AAV. Instead, doctors rely on a combination of symptoms, laboratory tests, biopsies, and imaging to confirm the diagnosis.
Symptoms that may lead to diagnosis
The first symptoms of AAV vary widely depending on which organs and tissues are affected, but may include:
- kidney symptoms: bloody or foamy urine
- lung symptoms: shortness of breath, coughing, severe asthma-like symptoms
- ear, nose, throat, and upper respiratory symptoms: sinus pain or congestion (the sinuses are air-filled spaces in the skull), nasal discharge or crusting, and ear pain
Other early signs of AAV are nonspecific but can still help guide doctors toward a diagnosis. These include:
- fatigue
- weight loss
- fever
- night sweats
- joint or muscle pain
Because manifestations of AAV in patients vary, it can be difficult to recognize separate symptoms as part of the same disease. By closely tracking symptoms, patients can help doctors more quickly suspect AAV.
In some cases, signs of AAV are detected through clinical tests done for other reasons, before a person develops obvious symptoms.
Blood tests
If a person’s symptoms suggest AAV, blood tests can help identify molecular markers linked to the disease. In many cases, self-reactive antibodies called ANCAs drive AAV immune activity by targeting one of two proteins — myeloperoxidase (MPO) or proteinase 3 (PR3).
An ANCA blood test can identify ANCAs and their target proteins, but it cannot confirm or rule out AAV on its own. Some people with AAV test negative for ANCAs, while others without AAV test positive.
Test results may also help doctors predict which type of AAV is present and what symptoms a person is more likely to develop.
Doctors may also order additional blood tests to look for:
- inflammatory or immune markers
- signs of kidney dysfunction
- possible infections or other autoimmune conditions
Urine tests may also be used when kidney involvement is suspected.
Imaging and biopsy procedures
To look for inflammation and damage consistent with AAV and to rule out other conditions with similar symptoms, doctors may use imaging scans and biopsies, in which tissue samples are examined under a microscope.
Imaging is used to assess organ involvement based on a person’s symptoms. Common AAV imaging tests include:
- CT or MRI scans
- X-rays
- endoscopies
CT, MRI, and X-rays can help visualize problems in tissues affected by AAV, including the lungs, heart, sinuses, brain, eyes, and abdominal organs. These scans can sometimes detect disease before symptoms appear.
Endoscopies involve inserting a thin tube with a camera into the body to examine hard-to-reach areas. For AAV, endoscopies are most often used to examine the airways, lungs, sinuses, or gastrointestinal tract.
Examining tissue samples under a microscope can reveal features of AAV or suggest another diagnosis. An AAV biopsy may be performed when doctors suspect damage to the kidneys, nerves, skin, or lungs. They are often collected during an endoscopy.
How diagnosis is confirmed
Because there are no standard diagnostic criteria for AAV, doctors must evaluate the full clinical picture and look for disease patterns. Symptoms, blood tests, imaging, and biopsies all play a role in how AAV is diagnosed.
It is also important to rule out other conditions that can mimic AAV, including:
- other types of blood vessel inflammation (vasculitis)
- bacterial, viral, or fungal infections
- cancer
- other autoimmune diseases, including lupus, IgG4-related disease, and sarcoidosis
Because many factors can complicate diagnosis, diagnostic delays are common, and multiple rounds of testing may be needed. Seeing a specialist with appropriate expertise can help ensure an accurate and timely diagnosis.
Understanding types of AAV
Confirming an AAV diagnosis also involves identifying the disease type, which helps guide treatment and monitoring strategies. There are three main AAV types:
- microscopic polyangiitis (MPA): most often associated with MPO-ANCA; commonly affects the kidneys, lungs, skin, or nerves
- granulomatosis with polyangiitis (GPA): most closely associated with PR3-ANCA; commonly affects the lungs, kidneys, nose, throat, and sinuses
- eosinophilic granulomatosis with polyangiitis (EGPA): the rarest AAV type, with about 60% of cases being ANCA-negative; commonly affects the lungs and upper respiratory system
In GPA and EGPA, clusters of immune cells called granulomas form at sites of inflammation, a feature not seen in MPA.
In 2022, the American College of Rheumatology and the European Alliance of Associations for Rheumatology published updated classification criteria for MPA, GPA, and EGPA. As scientists gain a better understanding of AAV, these criteria will likely continue to evolve.
Next steps after diagnosis
After diagnosis, an AAV specialist can help develop a treatment plan tailored to each patient. AAV prognosis tends to be better if treatment begins soon after diagnosis. Patients should continue to monitor their symptoms and promptly alert a healthcare provider if they notice any signs of new disease activity.
Adjusting to life with a chronic autoimmune condition can be challenging, so it’s important to find emotional and mental health support from friends, family, or other community members.
There are various support groups and educational resources available to help people adjust to life after an AAV diagnosis.
ANCA Vasculitis News is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website.
 Fact-checked by
Fact-checked by 

