Specific Eye Inflammation Seen as Early Sign of Granulomatosis with Polyangiitis in Case Study
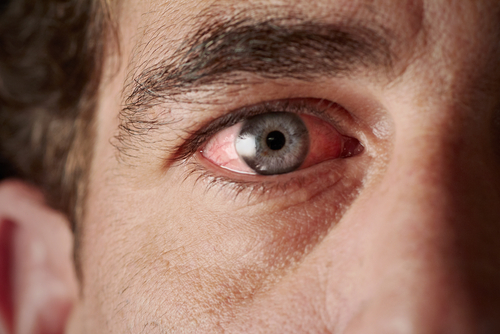
A case report finds that necrobiotic xanthogranuloma scleritis, an inflammation of the white part of the eye, could be an early sign of granulomatosis with polyangiitis.
The study, “Necrobiotic xanthogranuloma scleritis in a case of granulomatosis with polyangiitis (Wegener’s granulomatosis)” was published in the International Medical Case Reports Journal.
Scleritis is an inflammatory disease of the sclera (white of the eye), which could be associated with systemic inflammatory diseases such as rheumatoid arthritis, inflammatory bowel disease, relapsing polychondritis, systemic lupus erythematosus, polyarteritis nodosa, giant cell arteritis, and gout.
Scleritis sometimes occurs in cases of necrobiotic xanthogranuloma, which in itself is a rare chronic granulomatous disorder that presents as yellowish plaques and nodules. There is overlap between necrobiotic xanthogranuloma and granumolatosis with polyangiitis (GPA) in terms of clinical and histopathological findings. In fact, quite recently, a case diagnosed as GPA later turned out to be a case of necrobiotic xanthogranuloma with bilateral scleritis and orbital involvement.
The new case report described a case that would help to understand the relationship between GPA and necrobiotic xanthogranuloma.
The authors describe a 53-year-old man who presented with progressive visual loss and scleritis in his left eye, while his right eye was unaffected. The left eye was initially treated as infectious scleritis and endophthalmitis, but showed no improvement after two weeks of treatment. Tests for infectious agents were negative, including gram stain, bacterial, fungal and mycobacterial culture, herpes and tuberculosis.
The patient later suffered from prolonged fever and transient visual loss, and again no infections were detected, including HIV and hepatitis B and C. Heart, lung, and abdominal examinations were all normal. Biochemical tests were also generally normal.
However, anti-neutrophillic cytoplasmic antibodies (ANCA) were detected (C-ANCA and anti-PR3). Based on the presence of these antibodies and on granuloma found in the scleral tissue, the patient was diagnosed with GPA.
He was treated initially with high-dose corticosteroid and later with intravenous cyclophosphamide. As a result, systemic and eye conditions showed improvement and the patient responded well.
The authors conclude that “to the best of our knowledge, this case report first identified the relationship between necrobiotic xanthogranuloma scleritis and granulomatosis with polyangiitis. Early diagnosis of GPA is very important as it enables the appropriate treatments such as immunosuppressive therapy for reducing the risk of progression of the disease early and the involvement of other vital organs which could possibly deteriorate the prognosis dramatically.”
GPA, also known as Wegener’s, is among the group of autoimmune diseases collectively known as ANCA vasculitis and characterized by inflammation and destruction of small vessels.





