Eye Disease Affects About a Fifth of ANCA-associated Vasculitis Patients, Study Finds
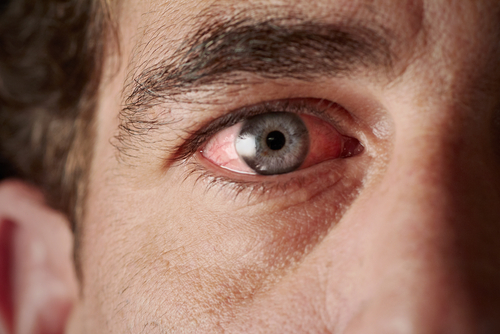
About a fifth of ANCA-associated vasculitis patients have an eye disorder known as inflammatory ocular disease, a Mayo Clinic study shows.
The research, published in the journal Rheumatology, was titled “Clinical characteristics of inflammatory ocular disease in anti-neutrophil cytoplasmic antibody associated vasculitis: a retrospective cohort study.”
ANCA-associated vasculitis, or AAV, affects a lot of systems, so those who have it can experience a wide range of symptoms. It can affect the lungs, kidneys, skin, paranasal sinuses, joints, peripheral nerves, and eyes.
Those with lung and kidney manifestations usually have a worse prognosis and a higher risk of death.
Many AAV patients have inflammatory ocular disease, which affects all parts of the eye and the eye socket, but no studies had assigned a patient-population percentage to it.
In addition, few studies have dealt with how the eye disorder develops or the outcomes of AAV patients who have it. And the studies that have been done involved only a small number of patients, which made it hard to draw conclusions from them.
Mayo Clinic researchers decided to do a more definitive study on the eye disease in AAV patients.
They first looked for potential cases of AAV among patients treated at the clinic between 2003 and 2013. Then they used the Chapel Hill Consensus Conference 2012 disease-description index to decide whether the patients had AAV, whose full scientific name is anti-neutrophil cytoplasmic antibody (ANCA)-associated vasculitis.
The next step was to look at whether patients diagnosed with AAV had inflammatory ocular disease, as well as patients’ symptoms, treatments and outcomes.
Among the 1,171 confirmed AAV cases, 183 patients, or 16 percent, had the eye disease. In half of the 183, the disorder was the primary symptom that led to an AAV diagnosis.
The most common manifestation of the ocular disorder was eye injection, a condition stemming from increased blood flow to the eyes. Fifty-seven percent of patients had this symptom. Forty-six percent had eye pain and 18 some loss of vision. About 40 percent of patients had the disease in both eyes.
There are several subtypes of inflammatory ocular disease. One is scleritis, which affects the sclera, or white outer coating of the eye. Another is episcleritis, which affects a thin layer on top of the sclera. Still another is socket inflammation. And there is also uveitis, or inflammation of the uvea, the middle layer of the eye.
Twenty-two percent of the patients with inflammatory ocular disease also had scleritis, 21 percent episcleritis, 18 percent socket inflammation, 10 percent lacrimal duct stenosis — or narrowing of the tear duct — and 9 percent uveitis.
Doctors used oral glucocorticoids to treat inflammatory ocular disease in 96 percent of the patients. In addition, 54 percent received the immunosuppressive agent cyclophosphamide and 36 percent another immunosuppressive agent, Rituxan (rituximab).
Fifty-two percent of patients with socket inflammation had surgery for it.
The various treatments worked well, with 91 percent of patients achieving remission of their condition for awhile. Twenty-three percent relapsed, however. And six patients ended up with major vision loss.
Another finding was that all of the patients with eosinophilic granulomatosis with polyangiitis and microscopic polyangiitis achieved remission, while only 89 percent of patients with granulomatosis with polyangiitis did so.
The eye disease “occurred in about one-fifth of patients with AAV,” the team said. “Scleritis, episcleritis and orbital [socket] inflammation were the most common subtypes” of the disease. “Response to treatment was generally satisfactory, with over 90 percent achieving clinical remission.”





